From Ebola to COVID-19: Lessons from DRC for improving community health responses
Following the devastating Ebola epidemic in Guinea, Liberia and Sierra Leone in 2013–16, the second Ebola outbreak in the Democratic Republic of Congo (DRC) in 2018 may seem like a whole other health crisis ago. But due to the coronavirus disease (COVID-19) and recent news of new Ebola outbreaks in Guinea and DRC, its lessons for effective health responses are more relevant now than ever.
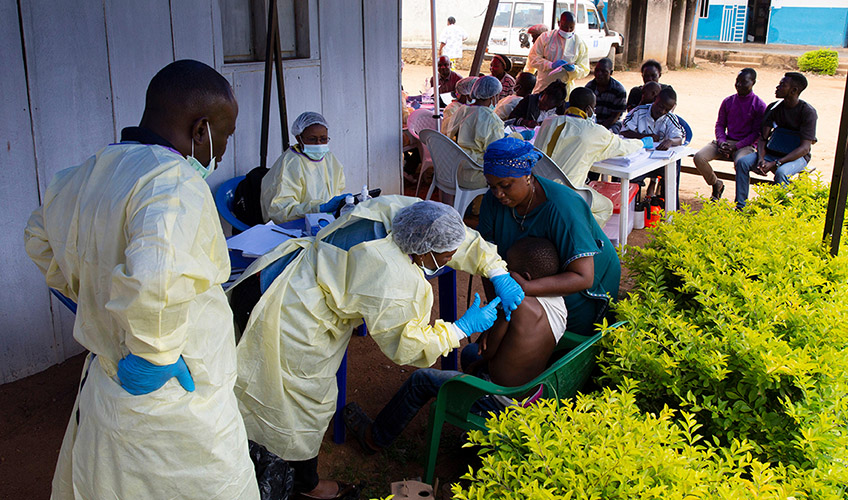
The Kivu Ebola epidemic officially began on 1 August 2018, when four cases of the Ebola virus were confirmed in the eastern region of Kivu in DRC. The two-year-long outbreak that followed resulted in 3,481 cases and 2,299 deaths, before the epidemic was finally declared over on 25 June 2020. During this period, the epidemic spread through the South Kivu, North Kivu and Ituri provinces of DRC, an active conflict zone with a public health system already crippled by the effects of a chronic humanitarian crisis.
A study conducted by International Alert DRC identifies a series of social, cultural and political factors that prevented the epidemic from being effectively controlled and managed by DRC’s government, the World Health Organization (WHO), and local and international partners. These structural factors limited the take-up of public health measures and, in some cases, led to violent attacks against Ebola response workers. The lessons from the study are discussed here and compared to the COVID-19 pandemic response to highlight correlations and the importance of incorporating these lessons into future public health responses.
Lack of trust
A key factor that restricted implementation of the health response in DRC was the lack of trust in government. The prevalence of armed groups in Kivu and Ituri, and the failure of government-led military operations to stop civilian massacres in the past, has resulted in a severe lack of confidence in the political establishment. This helped to fuel mistrust and legitimised hearsay that the government, local authorities and intervening international actors were somehow benefiting from the epidemic, with the phrase “Ebola business” entering widespread use.
This was compounded by the postponement of the 2018 election processes in Beni and Butembo, which identify as strong opposition heartlands within North Kivu. The decision was seen as a direct attack on democratic principles and processes, further fuelling the “Ebola business” rumours and increasing suspicion of authority figures. This drastically impaired the take-up of public health messages and measures.
Ebola was also perceived locally as an unknown, foreign disease, introduced to exterminate the locals and enrich humanitarian and government actors. This was exacerbated by a health response carried out by foreigners and Congolese from unaffected regions and led to many community members refusing to believe that Ebola was real. As a result, there was resistance and mistrust towards Ebola response teams, which significantly undermined implementation of the response.
Cultural clashes
The contrast between cultural practices and the prescribed health responses to Ebola made the situation even more difficult. Ancestral burial rights and compassionate community care for the sick are strong traditions in the Beni and Butembo regions and were severely disrupted by the Ebola restrictions. The relationship between communities and response workers who discouraged these cultural practices was partly defined by this cultural tension.
Traditional medicine also has a long history in DRC and is one of the most accessible and widely used healthcare options by a significant portion of the population. A perception that Ebola treatment centres and other care facilities were places of contagion and death led to people continuing to seek advice and medicine from traditional healers. Despite many new cases being traced to contact with a traditional healer or herbalist, or participation in traditional funerals, the trust in traditional medicine and suspicion of the Ebola treatment centres weakened the effectiveness of the response.
Local inclusion
At the onset of the epidemic, Ebola response workers assumed that the local capacity of staff and infrastructure was insufficient to deal with the epidemic. However, this overlooked local health workers and infrastructure, who have successfully dispensed vaccinations and controlled diseases for years and holds credibility in the local communities. Not incorporating this vital community link limited community ownership of the response and exacerbated communities’ mistrust of Ebola response teams.
As it is often needed for pragmatic reasons, emergency response relied on qualified people with previous experience of treating Ebola outbreaks, rather than on local capacity. As a result, local civil society leaders, customary and administrative authorities, religious leaders, local youth and others also spoke out about not being sufficiently involved in the response and complained that the local workforce did not have a prominent place in local interventions. Although this was justified to reduce the spread of the virus and save lives, greater consideration of these influential actors may have improved local and regional cooperation.
Lessons to learn
Responders learned that when there is no trust in or any perceived legitimacy of the medical profession, and no collaboration with communities, public health responses are impossible.
Building trust in the community requires greater transparency of monetary flows and decision-making procedures (locally, nationally and internationally), and clarifications of who is involved in the response and why.
More community leaders and influencers need to be engaged in the response as intermediaries between response teams and the community. For example, dignified and safe burial practices have divided the community response, but improved community dialogue could allow health workers and the community to find common ground. This can be facilitated through townhall meetings, dialogue processes and existing civil society structures, in addition to providing effective feedback and complaint mechanisms.
Responders must also ensure that the health response is participatory, inclusive, transparent and sensitive to gender and conflict dynamics.
Additionally, responders should look to adapt health responses to utilise local capacity and infrastructure where possible, with a focus on improving capacity. They should also advocate for basic hygiene measures that are familiar to people and emphasise prevention through these means. These adaptions should make responses easier to integrate and can align with community behaviours if they are rooted in local realities.
Response strategies should also consider the social, cultural, political and security context of intervention areas, based on regular analysis of the socio-security context. This will improve responders’ understanding of local complexities and help to further inform and adapt responses to the needs of the affected communities.
Responders should also offer free medical support and compensation for any material that is incinerated to prevent the spread of the virus, and they should support survivors to reduce stigma and facilitate their reintegration within communities. Without these protections, long-term economic and social impacts will seriously hinder community recovery.
Drawing parallels to COVID-19
Integrating these lessons into health responses has become more pressing in the wake of the ongoing COVID-19 pandemic, especially given some overt similarities between the two crises. Indeed, many of the reactions of Congolese communities towards the Ebola measures are mirrored in responses to COVID-19 preventative measures throughout Europe, the US and globally.
The lessons from DRC demonstrate how important it is to root responses in the local context, delivered through locally identifiable mechanisms and with local expertise, to build trust and compliance with the necessary health response.
Early in the COVID-19 pandemic, we saw how societies that can internalise the response through familiar procedures can rapidly adjust to new requirements, such as in China, Japan and South Korea, where memories of SARS and MERS are still fresh. And we saw how communities are best positioned to respond to local needs, with community leaders stepping up to provide for and protect their neighbours.
Improving access to information and increasing transparency of local, national and international spending and decision-making processes are also imperative towards enabling an effective health response. This is exemplified by the increased prevalence of governmental daily briefings during the COVID-19 pandemic and the level of scrutiny to which WHO and other decision-makers were held.
In addition, the economic impacts of health emergencies are highly pronounced and will be a residual effect of COVID-19 for the foreseeable future. While the long-term implications of different states’ economic measures are yet to be evaluated, it is evident that people’s livelihoods require protection during these times and that the financial burden of an emergency response should be borne by a government, not its people.
Given these parallels, it is imperative that health responders learn the lessons from the Kivu Ebola crisis. Chief among them is the importance of trust-building, cooperation and inclusion within local systems. These are not only vital lessons for responding to today’s pandemics and outbreaks; they could help improve our local and global resilience against future emergencies too.
About the project
International Alert, along with consortium partners Mercy Corps, Oxfam, CARE International and the Collectif des radios et télévisions communautaires du Nord-Kivu (CORACOM) implemented the project entitled ‘Lutter Contre Ebola via des Communautés Redynamisées’ (LEVER) between November 2019 and October 2020, in technical partnership with Viamo and Domagi, and with funding from USAID/OFDA.
As part of this project, a study was commissioned to identify lessons from the Ebola response in the Beni and Butembo regions of the Democratic Republic of Congo. You can read a summary of the study here. The full report is available upon request.







